Telehealth is Here to Stay: New 50 State Survey of Commercial Insurance Laws Reveals Progress
December 2, 2019

Two years after Foley’s 2017 Telemedicine and Digital Health Survey uncovered a demand for telemedicine and digital health services, as well as coverage and reimbursement to match the growing demand, Foley explores how each state has responded in its 2019 50-State Telehealth Survey plus District of Columbia (DC) of Commercial Payer Statutes.
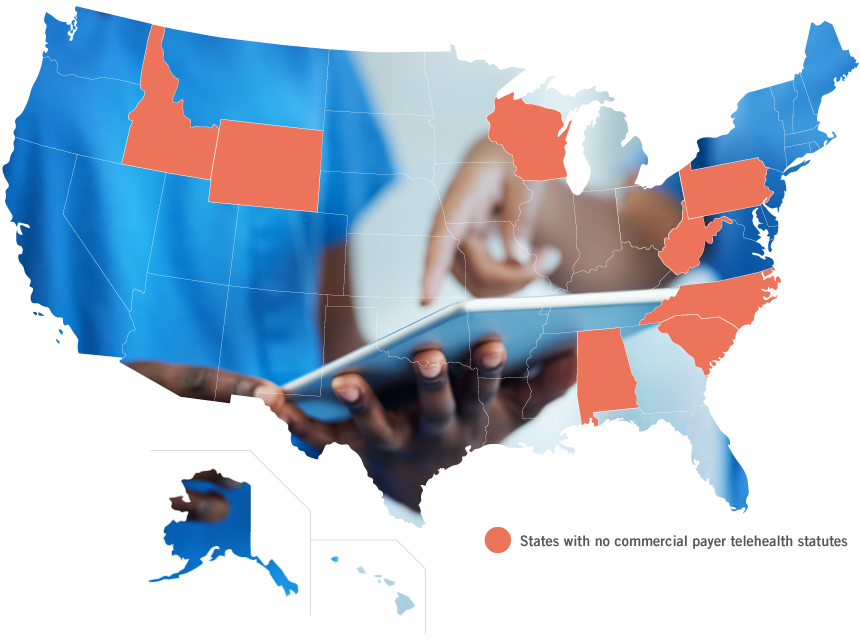
The survey found that as of October 2019, 42 states maintain some sort of telehealth commercial payer law, however several of these state laws do not actually require coverage or payment parity.
Foley’s report breaks down variances in telehealth commercial statues state-by-state, including:
- States that have commercial payer statutes in place
- States that have coverage parity or limitations
- States that have payment parity
- States that impose originating site limits
- States that have patient cost shifting protection
- State laws that address telehealth narrow or exclusive networking
- States that require coverage of reimbursement of remote patient monitoring
- States that require coverage of store & forward/asynchronous telemedicine
To read the full survey, download the 2019 report.
Author(s)
Related Insights
June 1, 2026
Energy Current
The Power Grid Passed Its Report Card. But Read the Fine Print.
What NERC’s 2026 Summer Reliability Assessment tells energy executives about where the power grid actually stands — and why the risks…
June 1, 2026
PharmaPatents
New USPTO “Pre-Docketing Notice” Pilot Program Could Streamline Examination
The USPTO announced a new pilot program that could streamline examination, improve examination efficiency, and help the USPTO use its examination resources more efficiently. The “Pre-Docketing Notice” pilot program also offers significant benefits to patent applicants, providing a timely opportunity to trim portfolios to save costs or align portfolios with current commercial objectives, which may have shifted in the years since the patent application was filed.
June 1, 2026
Health Care Law Today





